White paper
Beyond Survival: The Hidden Impact of Postpartum Hemorrhage
Maternal hemorrhage extends far beyond the delivery room.
Postpartum hemorrhage (PPH) is one of the leading causes of maternal morbidity and mortality globally, and a growing patient safety crisis in the United States. While advances in obstetric care have improved survival, the true impact of maternal hemorrhage extends far beyond the delivery room, affecting long-term maternal health, infant development, and broader societal outcomes.
The True Impact of Maternal Hemorrhage
Today, we often summarize maternal hemorrhage as a physical complication, but the impact of hemorrhage extends far beyond the physical, reaching throughout the first year of postpartum life and beyond.

Maternal Physical Health
Bleeding may stop, but recovery is often incomplete. Severe postpartum hemorrhage can result in persistent anemia, fatigue, and reduced functional capacity, limiting a mother’s ability to care for her newborn and regain stability in daily life. In more severe cases, ICU admission, transfusions, or surgical interventions, including hysterectomy, may be required. While lifesaving, these interventions can lead to long-term complications such as infection, chronic pain, and loss of fertility, further delaying recovery and disrupting early caregiving.
Maternal Mental Health
For many women, hemorrhage is not only a physical event, but a psychological one. The sudden, life-threatening nature of PPH can contribute to postpartum PTSD, depression, and anxiety. Symptoms such as intrusive memories, hypervigilance, and emotional distress may persist well beyond the birth experience, affecting maternal well-being, relationships, and confidence in caregiving.
Together, these consequences highlight an important reality: survival alone does not define recovery. The effects of postpartum hemorrhage extend well beyond the initial event, shaping a mother’s ability to heal, bond, and navigate early motherhood.
The Domino Effect: From Maternal Trauma to Societal Impact
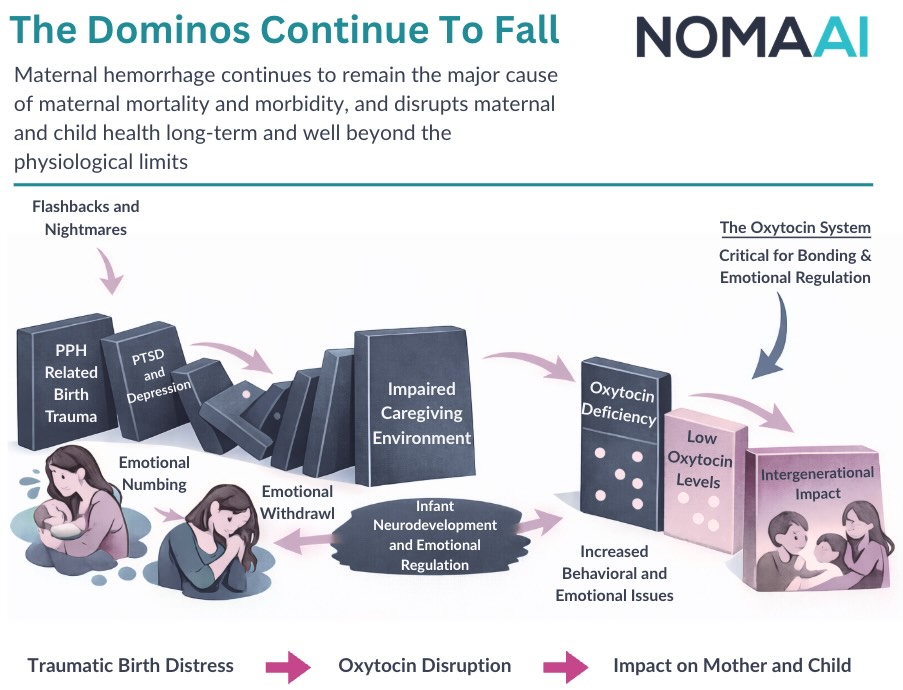
Postpartum hemorrhage sets off a cascading chain of consequences:
Maternal Complications → Disrupted Bonding → Infant Development Risks → Long-Term Child Outcomes → Societal Impact
- Interrupted breastfeeding and early bonding (“golden hour”)
- Impaired maternal-infant attachment
- Increased risk of behavioral and psychiatric disorders in children
- Higher exposure to adverse childhood experiences (ACEs)
- Family instability, financial strain, and reduced workforce participation
- Long-term societal burden through increased healthcare and social needs
PPH is not just a clinical event—it is a multi-generational health and economic issue.
Solutions & Opportunities
In this white paper, we explore the opportunity to make a significant impact and improve maternal and infant outcomes through:
- Advanced risk stratification and predictive analytics
- Real-time monitoring and early detection systems
- Clinical decision support tools
- Workflow-integrated care coordination technologies
- Data-driven quality improvement systems
- Postpartum monitoring and longitudinal care solutions
Additional Topics Covered
- Maternal-infant bonding and breastfeeding disruption
- Neurodevelopmental impact on infants
- Oxytocin regulation and stress biology
- Family and caregiver burden
- Economic and workforce implications
- Gaps in postpartum follow-up care
- Limitations of current hemorrhage detection methods
- Role of continuous monitoring and wearable technologies
- Importance of clinician-centered technology design
- Opportunities for proactive vs. reactive maternal care